2022 is picking up right where 2021 left off. At this point, we’ve used the word “unprecedented” so often that it has little meaning. At times, the path forward seems murky but amid difficulty there is opportunity.
Over the past year, I have witnessed great things from providers as they have rolled up their sleeves to ensure patients receive the proper care. To enable this success, hospital administrators have been forced to make hard decisions and find innovative solutions.
That innovation will continue in the new year as leaders address these 3 Trends for Healthcare Staffing.
Hybrid Telehealth Model
Telehealth is nothing new in healthcare. It has been seen as a potential disruptor to the traditional care model for a decade, but COVID-19 has expedited this change. The telehealth market size is already estimated at $55.9 billion and projected to grow to $431.82 billion by 2030.
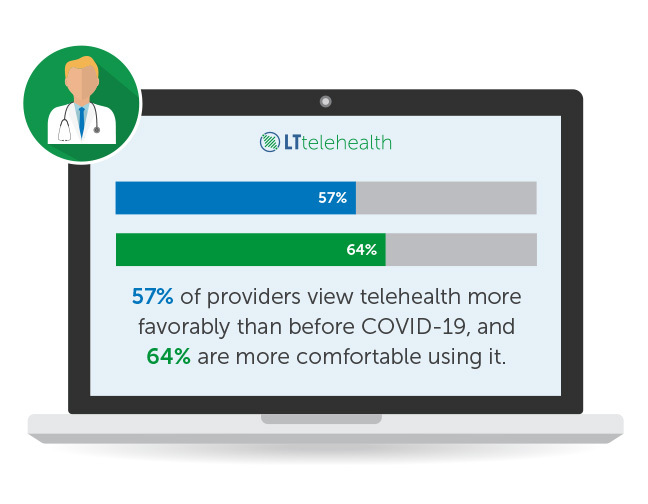
Survey data shows that consumers want to see more virtual options. On the physician side, as of April 2021, 84 percent of physicians offered virtual visits. Most said they would continue to provide these services long term. There has been a real shift in physician perception of telehealth services as providers were pushed to use virtual resources at the start of the pandemic. According to the American Hospital Association, 57 percent of providers view telehealth more favorably than before COVID-19 and 64 percent are more comfortable using it.
That only tells half the story.
Telehealth is an immensely valuable tool for a health system to provide value to patients, but in some circumstances an in-person care model is irreplaceable. In talking with clients, I’ve heard about the need for comprehensive, cost-effective solutions that increase access to care. Many have told me they are either looking at or starting to implement a hybrid telehealth model.
Leaders say a hybrid telehealth model that integrates virtual medicine with onsite care brings:
- Increased access to care
- Flexibility with staffing
- Efficiency improvement with staffing
- Reduced staffing costs
Among other benefits, hospitals will continue to explore a hybrid telehealth model in 2022 as they look to provide value during a challenging staffing environment.
Advanced Practice Professionals
With staffing resources remaining a challenge for health systems, finding new ways to deliver care and value can have a major impact on a health system. For the past few years, hospitals have embraced advanced practice professionals (APPs) and they will play an important role in 2022.
The Bureau of Labor Statistics predicts a 45 percent growth in APPs over the next decade. APPs can help to alleviate staffing challenges, while also providing a less expensive alternative to physician-only staffing. That will lead to new levels of efficiency and provide additional access to care.
Practice to the top of license—Too often APPs are underutilized. Going forward, hospitals will embrace the value of the role in the care continuum by allowing APPs to practice at the top of the license and make meaningful healthcare decisions. With the proper communication, training and trust, this frees up physicians to handle the healthcare procedures and diagnosis that only they can handle.
Value—Cost is a major concern for hospital administrators as they weigh delivery models and maintain services long term. APPs can play an important role in minimizing cost while still providing the high-level of care patients expect.
Solving the challenges in our current healthcare environment requires the ability to take a critical eye to the situation and resources available. APPs can be an invaluable resource to lower cost and ensure continuity of care.
Vaccine Mandates
Mandates around vaccines are a political hot potato. Healthcare organizations have long required certain vaccines for caregivers, but COVID-19 has hit a nerve with many in healthcare who have refused to get the vaccine.
Regardless of your stance on the vaccine, the adoption or dismissal of vaccine mandates is an issue that will greatly impact healthcare staffing in 2022. While most health systems initially mandated the vaccine for their staff, that changed toward the end of 2021 as several major healthcare systems (notably HCA Healthcare, Tenet Healthcare, AdventHealth and Cleveland Clinic) removed the vaccine requirement.
It all comes down to staffing concerns. Many surveys show that 90 percent of healthcare providers are vaccinated, but there remains a crucial group of providers who have not adhered to mandates. 36 percent of travel nurses surveyed reported they are not vaccinated. Of those, 25 percent said they would leave the nursing profession if forced to get the vaccine.
That is a very real impact for hospitals who are already struggling to adequately staff units. As a result, how hospitals handle vaccine mandates in 2022 will be a defining issue and set a precedent that may have long term effects.
2022 will be an important year for our healthcare system. Along with the challenges of a pandemic, we have been given an opportunity. By recognizing the path forward and prioritizing staffing, we will find new and innovative ways to care for patients. And we will do it together.

About the author
Chris Franklin
President
Chris Franklin serves as president of LocumTenens.com. With nearly two decades in healthcare and technology staffing experience, Franklin leads the LocumTenens.com team as they partner with clients to deliver innovative solutions that increase access to care and provide value to patients. He lives in Milton, Ga. with his wife and three daughters.





